What You Should Know
- The Market Burden: Gastrointestinal (GI) conditions affect one in five adults in the United States and generate a staggering $112 billion in annual healthcare spending. Furthermore, gastroenterology has the third longest wait time for specialists in the country.
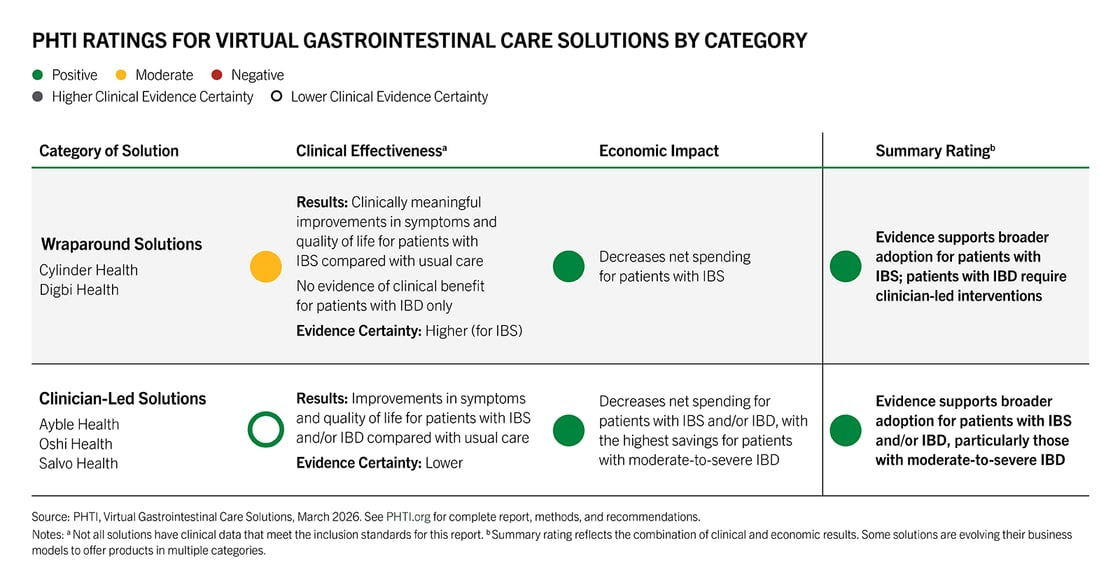
- The Assessment: In it’s latest report, The Peterson Health Technology Institute (PHTI) evaluated five virtual GI solutions: Ayble Health, Cylinder Health, Digbi Health, Oshi Health, and Salvo Health.
- Wraparound Solutions: Solutions like Cylinder and Digbi complement existing care with nutrition counseling, behavioral health, and symptom tracking. These deliver clinically meaningful improvements for patients with Irritable Bowel Syndrome (IBS). They substantially decrease net healthcare spending by $1,889 per year in the commercial market. However, there is no evidence of clinical benefit for patients with Inflammatory Bowel Disease (IBD).
- Clinician-Led Solutions: Solutions like Ayble, Oshi, and Salvo integrate a gastroenterologist and can prescribe and modify treatment plans. These solutions are effective alternatives to in-person care for IBD. The savings potential peaks when these solutions are targeted to patients with moderate-to-severe IBD, saving an estimated $2,901 per user on average.
The Great Divide: Wraparound vs. Clinician-Led
The most critical takeaway from the PHTI report is that not all GI platforms are built the same, and buying the wrong one for your specific patient population is a waste of capital. The market is split into two distinct categories:
1. Wraparound Solutions (Cylinder Health, Digbi Health) These platforms operate independently of a patient’s primary GI specialist, offering virtual support services like registered dietitians, mental health providers, and health coaches.
For patients suffering from Irritable Bowel Syndrome (IBS)—a functional disorder of the gut-brain interaction—these solutions are highly effective. By delivering gut-brain behavioral health and nutrition counseling, wraparound solutions achieve clinically meaningful symptom improvements. Better yet, they substantially decrease net healthcare spending for patients with IBS by $1,889 per year in the commercial market.
However, there is a catch. The limited available evidence examining wraparound solutions for patients with Inflammatory Bowel Disease (IBD) shows no clinical benefit over usual care. IBD causes visible, structural changes in the GI tract that require medical treatment, including specialty medications and surgery. A wraparound app simply isn’t enough to alter the course of structural tissue damage.
2. Clinician-Led Solutions (Ayble Health, Oshi Health, Salvo Health) This is where the heavy lifting happens. Clinician-led solutions offer a virtual multidisciplinary care model that directly integrates gastroenterologists into the platform. These clinical teams can develop and modify treatment plans, prescribe medications, and oversee the behavioral and nutritional support services.
Because these platforms can actually practice medicine, they appear to deliver comparable clinical outcomes to in-person multidisciplinary care for patients with IBD. While they come at a higher price point than wraparound apps, they drive massive ROI for high-acuity populations. The potential for savings is greatest when these solutions are targeted to patients with moderate-to-severe IBD, as well as those with IBS—saving an estimated $2,901 per user on average.
Aligning Payment with Reality
The PHTI data proves that virtual GI solutions hold immense promise, but purchasers must be highly strategic. If an employer’s workforce is primarily struggling with IBS, a lower-cost wraparound solution is a highly economical choice. But if a health plan is bleeding money on severe IBD flare-ups, hospitalizations, and biologics, they must invest in a clinician-led platform.
Furthermore, it is time to change how we contract for these digital health tools. Contracting should focus on clinically validated measurement and sustained reductions in hospitalizations or emergency department visits, rather than on proxy measures like enrollment or app usage. Performance-based contracts that tie payment to incremental improvements in clinical outcomes or reductions in utilization may better reflect the value delivered by virtual GI solutions.
“The clinical improvements from virtual GI solutions are meaningful for patients managing these chronic conditions that disrupt daily life,” said Caroline Pearson, Executive Director of PHTI. “These solutions can also produce valuable cost savings by improving symptom management and avoiding flare-ups that often lead to emergency department visits, testing, and hospitalizations.”


